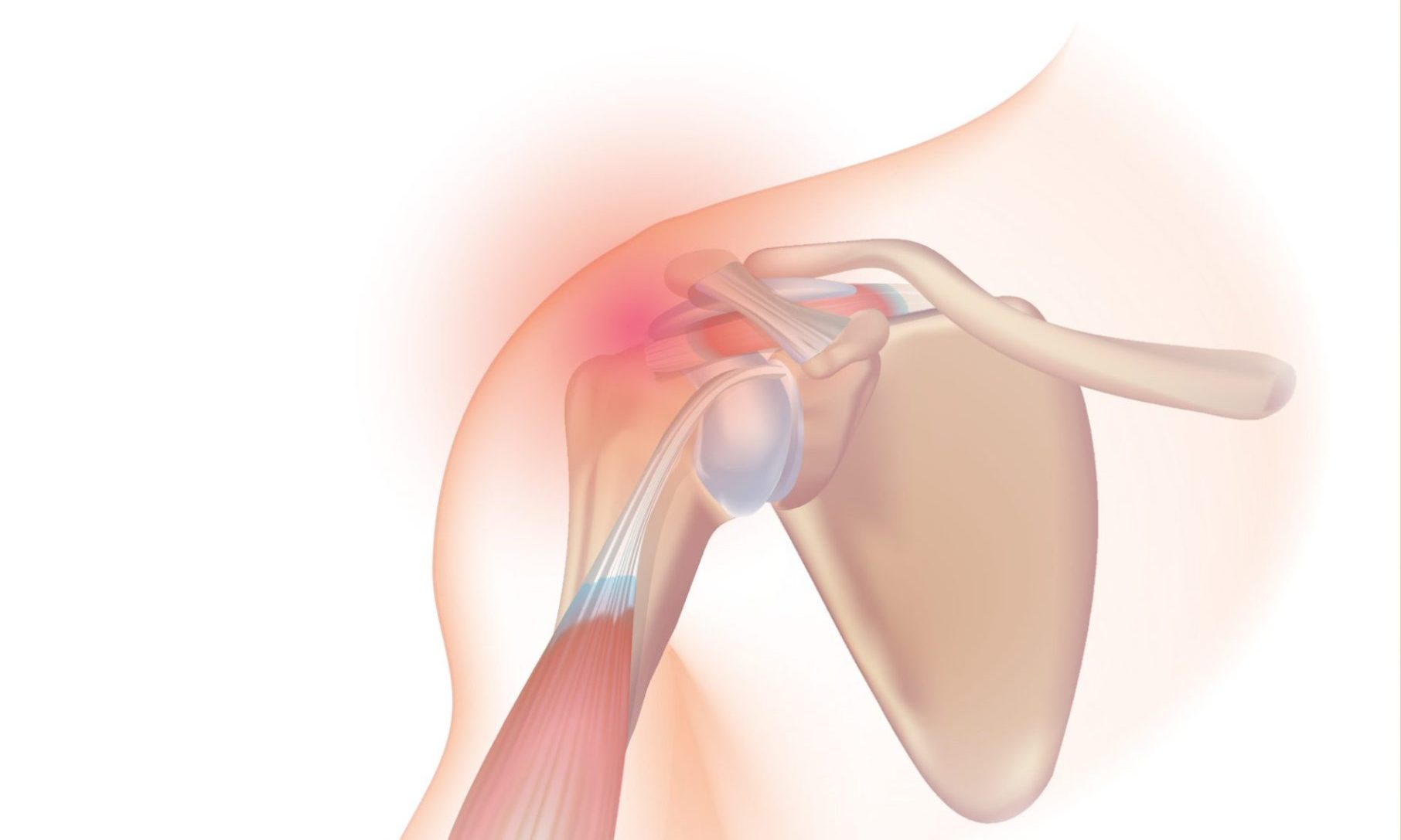
Adhesive capsulitis, also known as frozen shoulder, is a condition characterized by pain, stiffness, and limited range of motion in the shoulder joint. It occurs when the tissues surrounding the shoulder joint become thickened and tight, leading to a loss of mobility and function. Recovery from adhesive capsulitis is often a “slow burn” with the rehabilitation process typically spanning several months to greater than a year. Physiotherapy plays a crucial role in the management and rehabilitation of adhesive capsulitis, helping individuals regain shoulder mobility, have reduced pain, and improved function.
The treatment of adhesive capsulitis typically follows the 5 stages of rehab, which are designed to address pain, restore range of motion, improve motor control, strengthen the shoulder muscles, and maintain the gains achieved.
- Pain and symptom management: The initial focus is on relieving pain and reducing inflammation in the shoulder joint. Physiotherapists may use various modalities such as heat or cold therapy, manual therapy, joint mobilizations, dry needling, or gentle exercises to help alleviate pain during this stage.
- Range of motion: The next stage involves restoring and improving shoulder range of motion. Physiotherapy interventions may include passive range of motion exercises, with the therapist manipulating the shoulder joint to stretch the tight tissues. Active range of motion exercises are then introduced to encourage individuals to move their shoulder within pain-free limits. Gradually, the range of motion exercises progress to stretching techniques that target the affected structures and help increase flexibility. Stretches can often be provocative in the early phases of Adhesive Capsulitis, if this is the case, rehabilitation may progress to stages 3 and 4 before full range of motion is regained; returning to stage 2 when the shoulder joint is less irritable and likely to respond better to stretching.
- Motor control: In this stage, the focus is on enhancing neuromuscular control and stability around the shoulder joint. Physiotherapists design exercises that target the shoulder muscles and scapular stabilizers to improve muscle strength, control, and coordination. Proprioceptive training and specific exercises that challenge balance and coordination may also be incorporated to improve motor control and joint stability.
- Strengthening: Once pain and range of motion have improved, the emphasis shifts to strengthening the muscles around the shoulder joint. Physiotherapy exercises may include resistance training using bands, weights, or bodyweight to target the rotator cuff muscles, deltoids, and scapular stabilizers. Strengthening these muscles helps to support the shoulder joint, improve function, and prevent future injuries.
- Maintenance: The final stage focuses on maintaining the gains achieved throughout the rehabilitation process and preventing the recurrence of adhesive capsulitis. Physiotherapists provide guidance on an appropriate exercise program, incorporating regular stretching and strengthening exercises into daily routines. They may also advise individuals on proper posture, body mechanics, and modifications for activities that may place stress on the shoulder joint.
In addition to the 5 stages of rehab, recovery from adhesive capsulitis may involve other interventions such as shockwave therapy, injections or even surgery. Your Range Physio can help guide you when exploring whether these options will be beneficial or necessary. It’s important to note that the management of adhesive capsulitis requires patience and consistency. The duration of treatment can vary from months to greater than a year, depending on the individual and their response to therapy. Range Physios work closely with their patients to monitor progress, adjust treatment plans as needed, and provide ongoing support and guidance throughout the rehabilitation journey.
For more information regarding adhesive capsulitis please visit: